PERFORMER HTThe most advanced system for Hyperthermic Perfusion
All treatment data and events are automatically saved on a USB memory and with a proprietary excel based software a report of the treatment can be created in few minutes.
Right at the end of the treatment, a printout of the treatment data can be attached to the medical records.
The integrated UPS allows to continue the treatment also in case of power failure.
Power supply
110/230V – 50/60Hz
Power adsorption
Max 700VA
Electrical classification
Class I – Type BF
Protection IP
IP 21
Flow rates
2 peristaltic pumps ranging from 100 to 2000 ml/min
Pressures
6 pressure sensors ranging from -450 to + 450 mmHg
Volumes
Load cell ranging from 0.5 to 20 liters
Temperature
Plate warming system (28 to 46°C)
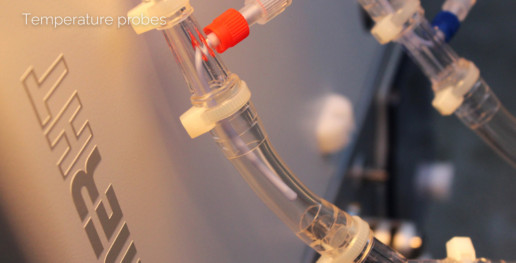
Monitoring through 8 external temperature probes
Dimensions (WxDxH)
500x550x960 mm (stand-by/transport mode)
500x550x1600 mm (operative conditions)
Weight
80 kg
Safety standards
UL 60601-1
General requirements for basic safety and essential performance
IEC 60601-1-2
General requirements for safety: Electromagnetic compatibility
IEC 62304
Medical device software – Software lifecycle processes
IEC 62366
Application of usability engineering to medical devices